Bell’s Palsy, a condition named after the Scottish anatomist Sir Charles Bell, is a neurologic disorder that affects the facial nerve, resulting in sudden paralysis or weakness on one side of the face. This condition, although temporary in most cases, can be a source of great concern and discomfort for those affected. Understanding the symptoms, causes, and recovery process of Bell’s Palsy is crucial for both patients and healthcare providers to ensure timely diagnosis, appropriate treatment, and a positive outcome. In this blog, we will delve into the intricacies of Bell’s Palsy, exploring its symptoms, potential causes, diagnostic methods, treatment options, and the journey of recovery for individuals facing this challenge.
In This Blog:
- Symptoms of Bell’s Palsy
- Causes of Bell’s Palsy
- Diagnosis of Bell’s Palsy
- Treatment Options
- Recovery and Prognosis
Symptoms of Bell’s Palsy
Bell’s Palsy presents with a range of symptoms that primarily affect the facial muscles and nerves on one side of the face. These symptoms can vary in severity and may include:
Facial Paralysis:
One of the hallmark symptoms of Bell’s Palsy is sudden weakness or paralysis of the facial muscles on the affected side. This can cause drooping of the eyebrow, eyelid, and corner of the mouth, resulting in an asymmetrical facial expression.
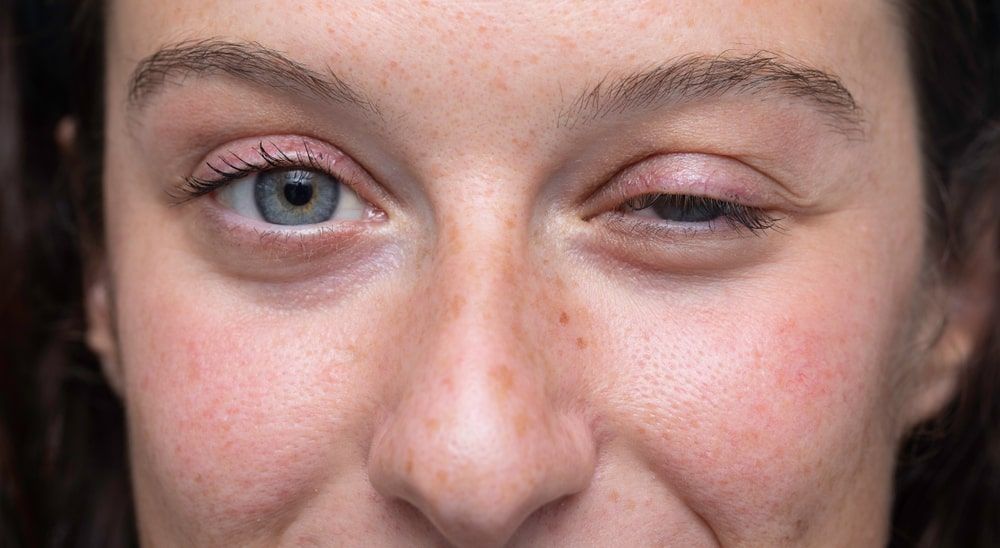
Difficulty Closing One Eye:
Due to the weakness of the facial muscles, individuals with Bell’s Palsy may experience difficulty fully closing one eye. This can lead to dryness, irritation, and increased sensitivity to light in the affected eye.
Loss of Taste:
Some individuals may notice a decreased or altered sense of taste on the side of the tongue corresponding to the affected facial nerve. This can affect their enjoyment of food and beverages.
Changes in Tear and Saliva Production:
Bell’s Palsy can disrupt the normal function of tear and saliva glands on the affected side of the face. This may result in dry eyes, excessive tearing, or difficulty producing saliva, leading to dry mouth and difficulties with speech and swallowing.
Recognizing these symptoms early and seeking medical attention is crucial for proper diagnosis and management of Bell’s Palsy.
Causes of Bell’s Palsy
Bell’s Palsy is believed to be primarily caused by viral infections, particularly the herpes simplex virus (HSV), although the exact mechanism is not fully understood. Other potential causes and risk factors include:
Viral Infections:
The herpes simplex virus, which is responsible for cold sores and genital herpes, is often associated with Bell’s Palsy. It is thought that viral replication and inflammation of the facial nerve may contribute to the development of the condition. Shingles may also contribute to the conditions.
Inflammation and Swelling:
In addition to viral infections, inflammation and swelling of the facial nerve (cranial nerve VII) can occur, leading to compression and dysfunction. This inflammatory response may be triggered by various factors, including infections, autoimmune reactions, and environmental factors.
Risk Factors:
Certain individuals may be at a higher risk of developing Bell’s Palsy. These risk factors include diabetes mellitus, pregnancy (especially during the third trimester and immediately postpartum), upper respiratory infections, and a history of previous Bell’s Palsy episodes.
While viral infections, particularly HSV, are considered the primary trigger for Bell’s Palsy, the interplay of inflammatory processes and individual predisposing factors plays a complex role in the onset and progression of this condition. Understanding these underlying mechanisms is essential for effective management and prevention strategies.
Diagnosis of Bell’s Palsy
Diagnosing Bell’s Palsy involves a comprehensive assessment of symptoms, medical history, and specialized tests to rule out other potential causes of facial paralysis. The diagnostic process typically includes:
Physical Examination:
A healthcare provider will conduct a thorough physical examination, focusing on the facial muscles, nerve function, and related symptoms. They may assess facial symmetry, eye movements, ability to close the eyes tightly, and strength of facial expressions.
Neurological Tests:
Neurological tests, such as the facial nerve conduction test (electromyography or EMG), may be performed to evaluate the function and response of the facial nerve. This test measures electrical activity in the facial muscles, helping to assess nerve damage and severity of paralysis.
Imaging Studies:
In some cases, imaging studies such as magnetic resonance imaging (MRI) or computed tomography (CT) scans may be recommended to rule out other underlying conditions, such as stroke, tumors, or structural abnormalities affecting the facial nerve.
The combination of clinical assessment, neurological testing, and imaging studies allows healthcare providers to make an accurate diagnosis of Bell’s Palsy and develop an appropriate treatment plan tailored to the individual’s needs. Early diagnosis is key to initiating timely interventions and maximizing the chances of recovery.
Treatment Options
Treatment for Bell’s Palsy aims to reduce inflammation, restore nerve function, and alleviate symptoms. The approach to treatment may vary depending on the severity of symptoms and individual factors. Common treatment options include:
Medications:
- Steroids: Oral corticosteroids, such as prednisone, are often prescribed to reduce inflammation and swelling of the facial nerve. Early initiation of steroid therapy within the first few days of symptom onset is typically recommended to improve outcomes.
- Antiviral Drugs: In cases where a viral infection, such as herpes simplex virus (HSV), is suspected or confirmed, antiviral medications may be prescribed to suppress viral replication and reduce nerve damage.
Physical Therapy:

- Facial Exercises: Physical therapy techniques, including facial exercises and massage, may be recommended to improve muscle strength, mobility, and coordination on the affected side of the face.
- Electrical Stimulation: Some individuals may benefit from electrical stimulation therapies, such as transcutaneous electrical nerve stimulation (TENS), to enhance nerve function and stimulate facial muscle contractions.
Eye Care:
- Eye Drops: Lubricating eye drops or ointments may be prescribed to prevent dryness and protect the cornea in cases where blinking and eye closure are impaired.
- Eye Patches: Temporary use of an eye patch may be necessary to protect the affected eye, especially during sleep, to prevent corneal abrasions and irritation.
Surgery:
In rare cases of severe or persistent facial nerve damage, surgical interventions such as facial nerve decompression or nerve grafting may be considered to restore facial symmetry and function. However, surgical options are typically reserved for refractory cases that do not respond to conservative treatments.
The choice of treatment modalities and the duration of therapy will be determined based on individual patient assessment, symptom severity, and response to initial interventions. Close monitoring and follow-up with healthcare providers are essential to track progress, adjust treatment plans as needed, and optimize outcomes for individuals with Bell’s Palsy.
Recovery and Prognosis
The recovery process for Bell’s Palsy can vary widely among individuals, ranging from spontaneous improvement to persistent symptoms requiring long-term management. Understanding the factors influencing recovery and prognosis is essential for patients and healthcare providers. Key points to consider include:
Spontaneous Recovery:
In many cases, Bell’s Palsy resolves spontaneously without specific treatment within a few weeks to months. The majority of individuals experience noticeable improvement in facial muscle strength and function within the first few weeks of onset.
Timeframe for Improvement:
The rate of recovery and degree of improvement can vary. Some individuals may experience rapid improvement within days, while others may have a more gradual recovery over several weeks to months. Patience and consistent adherence to treatment recommendations are important during the recovery process.
Potential Long-Term Effects:
While most individuals with Bell’s Palsy recover fully without significant long-term effects, some may experience residual symptoms or complications. These may include persistent facial asymmetry, weakness, or stiffness, as well as changes in taste sensation or tear production. Rehabilitation strategies and ongoing follow-up care may be necessary to address these challenges and optimize outcomes.
Factors influencing the prognosis of Bell’s Palsy include the severity of initial symptoms, age of onset, underlying health conditions, and promptness of treatment initiation. Early diagnosis, appropriate medical interventions, and supportive care play key roles in facilitating recovery and minimizing potential complications. It’s important for individuals with Bell’s Palsy to work closely with their healthcare team to monitor progress, address concerns, and develop a comprehensive plan for recovery and long-term management.
Conclusion
In conclusion, Bell’s Palsy is a neurologic condition characterized by sudden facial paralysis or weakness, often attributed to viral infections and inflammatory processes affecting the facial nerve. While the symptoms of Bell’s Palsy can be distressing, timely diagnosis, appropriate treatment, and supportive care can significantly improve outcomes and facilitate recovery. With a combination of medications, physical therapy, eye care, and in rare cases, surgical interventions, individuals with Bell’s Palsy can experience a gradual restoration of facial function and quality of life. It’s essential for patients, caregivers, and healthcare providers to work collaboratively to navigate the challenges of Bell’s Palsy, promote optimal recovery, and ensure long-term well-being.

Dr. Kashouty, a diplomate of the American Board of Psychiatry and Neurology (ABPN), practices general neurology with fellowship trained specialization in clinical neurophysiology. Dr. Kashouty finds the form and function of the nerves and muscles the most interesting part of neurology, which is what led him to specialize in neurophysiology with more emphasis on neuromuscular conditions. He treats all neurological diseases, but his main focus is to treat and manage headaches, movement disorders and neuromuscular diseases.




