With the start of 2022 we are entering the third year of the Coronavirus pandemic. Although coronaviruses, including the novel SARS-CoV-2 virus responsible for COVID-19, primarily cause mild to moderate upper respiratory problems, they can indirectly affect other areas of the body as well. This is generally due to a lack of oxygen in the blood, which severely impairs the body’s ability to function properly. As a result, COVID-19 can have an effect on the nervous system despite the fact that it is a respiratory illness. In this blog post, we will review how coronavirus affects the nervous system, its immediate effects on the brain, and what long-term neurological complications can occur after the virus has passed.
How Coronavirus “Infects” the Nervous System
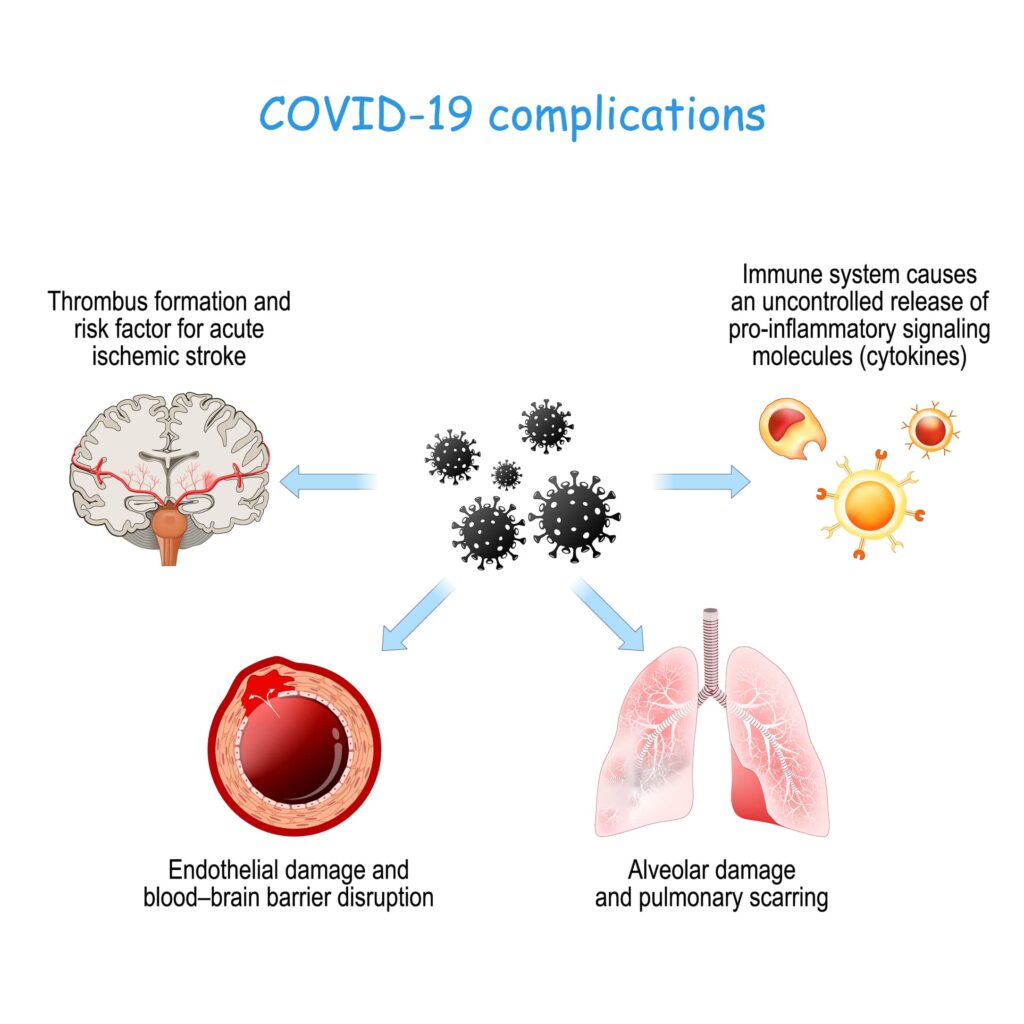
It is important to note that the relationship between COVID-19 and the nervous system is still being actively researched, which means assertions can change as new information emerges. With that being said, the current research shows that the SARS-CoV-2 virus primarily affects the nervous system through the immune system. Research shows that COVID-19 can cause the immune system to overreact. This is also sometimes known as a cytokine storm.
Cytokines are signaling molecules that are used by the immune system to fight infections. There are different types of cytokines with functions such as: recruiting immune cells, producing antibodies, signaling pain, clotting the blood, producing inflammation, and decreasing inflammation. During a cytokine storm, the cytokines that produce inflammation (inflammatory cytokines) outnumber the cytokines responsible for decreasing inflammation. This essentially causes inflammation to storm out of control, which often causes more harm than good.
During a cytokine storm, there are higher levels of cytokines in the blood. These changes in the blood also affect the cerebrospinal fluid that surrounds the brain and spinal cord. Although there is currently no evidence that shows the virus spreading through the brain, research is finding that these changes in the blood and cerebrospinal fluid can potentially cause reactions with the nervous system.
Immediate Effects of COVID-19 on the Brain
To understand how COVID-19 immediately affects the brain, we must have a brief understanding on how the virus works. The SARS-CoV-2 virus attaches to receptors on specific cells in the body. These specialized receptors are primarily found in the lung cells, however they are also found in the cells that line the blood vessels known as endothelial cells. As a result, COVID-19 can cause the blood vessels to become weak, leaky, or inflamed. COVID-19 can also cause blood clots or blockages within the blood vessels that restrict the normal flow of blood, oxygen, and nutrients, which can lead to stroke or heart attacks.
Even in cases where COVID-19 does not cause strokes or heart attacks, blood clots in or around the lungs can impede the flow of oxygen and cause hypoxia. Hypoxia, or low levels of oxygen in the blood, is highly damaging to the brain and other organs.
Most people with mild cases of COVID-19 do not experience neurological symptoms, however those with moderate cases requiring hospitalization usually experience one or more of the following neurological symptoms:
- muscle aches
- headaches
- dizziness
- alterations in taste or smell
In rare cases, COVID-19 can also cause strokes, seizures, muscular weakness, nerve injury, pain syndromes, and certain disorders of inflammation in the nervous system such as: Guillain-Barre syndrome, transverse myelitis, and acute necrotizing leukoencephalopathy.
Long-Term Neurologic Effects of COVID-19
Most people who experience mild to moderate symptoms are able to recover within a few days or weeks without any lasting effects. However, others with mild to moderate symptoms experience dysfunction of body systems and/or new symptoms as a result of the initial infection. Those who experience severe symptoms are at a much higher risk of experiencing continued body system dysfunction and/or the development of new symptoms. This is sometimes called Post Acute Sequelae of SARS-CoV-2 Infection (PASC), long COVID, or long haul COVID.
Some of the long-term neurological effects of COVID-19 include:
Nerve Damage
Peripheral neuropathy is a form of damage to the peripheral nervous system. The peripheral nervous system consists of pathways that carry signals from the brain and spinal cord to all parts of the body (arms, legs, hands, feet), as well as those pathways carrying information back to the central nervous system (brain and spinal cord) from the rest of the body. Peripheral neuropathy can lead to various symptoms, depending on the type of nerve affected.
Motor nerves are responsible for muscle movement and symptoms affecting the motor nerves can include muscle weakness and cramps. Sensory nerves are responsible for sending signals about sensations, temperature, pain, and other information from all parts of the body. Symptoms affecting the sensory nerves can include tingling or numbness in the hands or feet. Autonomic nerves are responsible for certain automatic functions of our body that occur without us thinking about them. They control things like heart rate, blood pressure, digestion, urination, sweating, and sexual function. Symptoms affecting the autonomic nerves can include dizziness upon standing or slow heart rates.
Fatigue
Fatigue is a feeling of exhaustion or tiredness. It often occurs after any type of viral infection, and the severity can vary. In some cases, fatigue after COVID-19 can be attributed to complications such as a decrease in heart, lung, or kidney function. In other cases, the exact cause of fatigue is not known.
Cognitive Impairment
Cognitive impairment associated with COVID-19 can include difficulty concentrating, memory problems, or a general sense of brain fog. In many cases, cognitive impairment is accompanied by some degree of fatigue. Immune, metabolic, or blood vessel abnormalities can be responsible for contributing to cognitive impairment, as can certain drugs used to treat the infection.
Pain

Many people have reported joint and muscle pain that lingers after the virus. People who had acute respiratory distress syndrome (ARDS), as well as some with mild or moderate infections, also report persistent chest pain.
Loss of Smell or Taste
The SARS-CoV-2 virus infects the tissues that line the inside of the nose, which are partially responsible for detecting odors and sending sensory information to the brain. When these cells become damaged, this causes a loss of smell and/or taste. As the cells repair themselves or are replaced by new cells, this can cause certain things to smell differently than before. Some people even note that certain things take on an unpleasant smell.
Headaches
Headaches can occur during and after the COVID-19 infection. In some cases, mild to severe headaches are reported for weeks following the initial virus. Some people have daily headaches, while others are infrequent. Headaches associated with COVID-19 differ from migraines, but generally have a 24/7 baseline that sometimes increases.
Sleep Problems
Sleep problems can occur as a result of long-term neurological effects or independently. After COVID-19, some people report trouble falling or staying asleep (insomnia), excessive daytime sleepiness (hypersomnia), and a general change in sleep patterns that can make it difficult to sleep or wake at certain times. Unfortunately, sleep deprivation can also cause other neurological symptoms to increase.
Mood Disorders
The stress caused by a COVID-19 infection can have varying effects on an individual’s mental health. Some people may develop depression, anxiety, or even post-traumatic stress disorder in some cases. The risk for these mood disorders generally increases depending on the severity of the infection, as well as the extent of medical treatment performed during hospitalization.
In Conclusion
As we have seen, coronavirus can have a significant effect on the nervous system. This is due to both the direct and indirect effects of the virus on the body. The immediate effects of COVID-19 on the brain can be devastating, leading to long-term neurological complications in some cases. It is therefore important that everyone takes precautions against contracting this virus, especially those who are at risk for serious health complications. If you have had COVID-19 and are still experiencing neurological symptoms, call our office today for more information.

Dr. Kashouty, a diplomate of the American Board of Psychiatry and Neurology (ABPN), practices general neurology with fellowship trained specialization in clinical neurophysiology. Dr. Kashouty finds the form and function of the nerves and muscles the most interesting part of neurology, which is what led him to specialize in neurophysiology with more emphasis on neuromuscular conditions. He treats all neurological diseases, but his main focus is to treat and manage headaches, movement disorders and neuromuscular diseases.





