Myasthenia Gravis (MG) is a chronic autoimmune neuromuscular disorder that disrupts communication between nerves and muscles, leading to muscle weakness and fatigue. This condition can affect various muscle groups, making everyday tasks such as speaking, swallowing, and even breathing more challenging. While there is no cure for MG, effective management through a combination of neurological treatments and lifestyle adjustments can significantly improve quality of life. From medications and advanced therapies to energy conservation techniques and dietary modifications, a well-rounded approach can help individuals with MG maintain their independence and well-being. In this blog, we will explore the latest treatment options and practical lifestyle strategies for managing Myasthenia Gravis effectively.
In This Blog:
- Understanding Myasthenia Gravis
- Neurological Treatments for Myasthenia Gravis
- Lifestyle Adjustments to Manage Myasthenia Gravis
- Preventing and Managing Myasthenic Crisis
Understanding Myasthenia Gravis
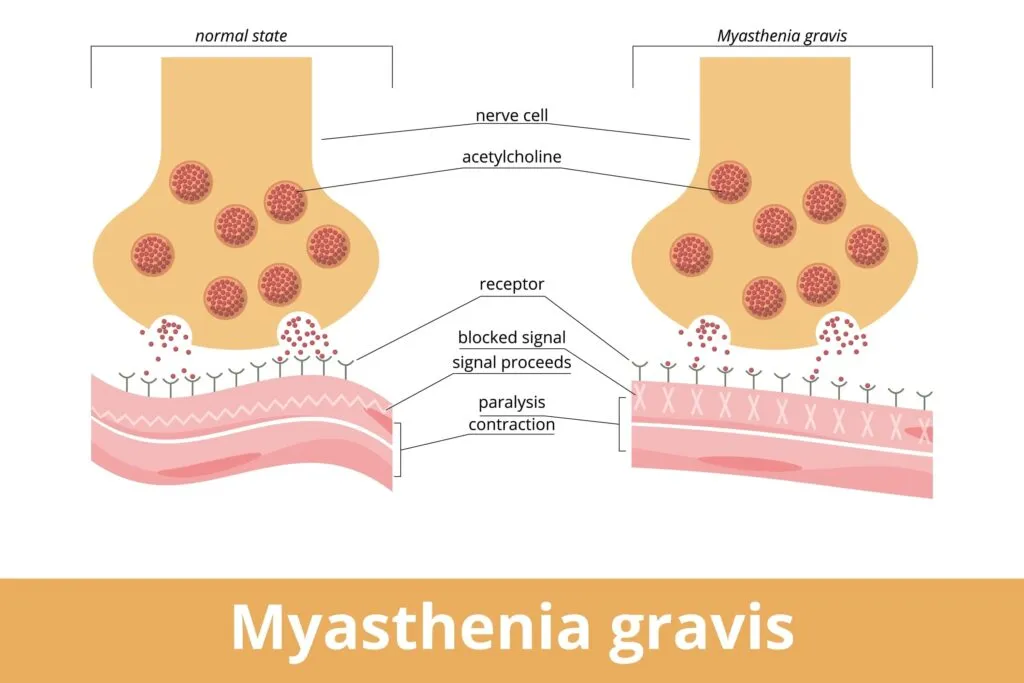
Myasthenia Gravis (MG) is a chronic autoimmune disorder that affects the neuromuscular junction, where nerve signals are transmitted to muscles. In individuals with MG, the body’s immune system mistakenly produces antibodies that block or destroy acetylcholine receptors, preventing proper muscle contraction. This disruption leads to the hallmark symptom of MG: muscle weakness that worsens with activity and improves with rest.
Common Symptoms of Myasthenia Gravis
The symptoms of MG can vary in severity and may affect different muscle groups. Some of the most common symptoms include:
- Muscle Weakness and Fatigue: Weakness that intensifies with repeated muscle use, often affecting voluntary muscles.
- Drooping Eyelids (Ptosis): One of the earliest and most noticeable signs, causing difficulty in keeping the eyes open.
- Double Vision (Diplopia): Weakness in the muscles controlling eye movement, leading to blurred or double vision.
- Difficulty Swallowing (Dysphagia) and Speaking (Dysarthria): Weakness in throat muscles, making it harder to chew, swallow, and articulate words.
- Shortness of Breath: In severe cases, MG can impact the muscles responsible for breathing, leading to respiratory distress.
How Myasthenia Gravis is Diagnosed
Diagnosing MG requires a thorough evaluation by a neurologist, including a combination of clinical assessments and specialized tests:
- Neurological Examination: A doctor will assess muscle strength, reflexes, and fatigue patterns.
- Antibody Testing: Blood tests can detect anti-acetylcholine receptor (AChR) antibodies or muscle-specific kinase (MuSK) antibodies, which are commonly associated with MG.
- Electromyography (EMG): A test that evaluates electrical activity in muscles to detect abnormal neuromuscular transmission.
- Edrophonium Test: A short-acting medication (edrophonium chloride) is administered to temporarily improve muscle strength, helping confirm the diagnosis.
- CT or MRI Scan: Imaging studies may be used to check for thymoma, a tumor of the thymus gland, which is sometimes linked to MG.
Understanding the causes, symptoms, and diagnostic methods of MG is essential for early detection and proper management. Once diagnosed, patients can explore available treatments and lifestyle adjustments to manage their condition effectively.
Neurological Treatments for Myasthenia Gravis
Managing Myasthenia Gravis (MG) requires a comprehensive approach that includes medications, advanced therapies, and sometimes surgical interventions. While there is no cure for MG, these treatments help improve muscle function, reduce symptoms, and prevent complications such as myasthenic crisis. The treatment plan is typically tailored to each patient’s specific symptoms, severity, and overall health condition.
Medications for Myasthenia Gravis
Several types of medications are commonly used to manage MG:
- Acetylcholinesterase Inhibitors: These medications, such as pyridostigmine (Mestinon), work by increasing the availability of acetylcholine at the neuromuscular junction, temporarily improving muscle strength. While effective for symptom relief, they do not treat the underlying immune dysfunction.
- Corticosteroids: Prednisone and other steroids help suppress the immune system and reduce antibody production that interferes with nerve-muscle communication. Long-term use may lead to side effects such as weight gain, osteoporosis, and high blood sugar.
- Immunosuppressants: Medications such as azathioprine (Imuran), mycophenolate mofetil (CellCept), and cyclosporine help reduce immune system activity, decreasing the severity of MG symptoms. However, they may take months to become fully effective.
Plasmapheresis and Intravenous Immunoglobulin (IVIG)
For patients with severe MG symptoms or those experiencing a myasthenic crisis (a life-threatening condition involving severe muscle weakness and respiratory failure), more aggressive treatments may be necessary:
- Plasmapheresis (Plasma Exchange): This procedure removes harmful antibodies from the blood and replaces them with healthy plasma or a plasma substitute. It provides short-term relief but requires multiple sessions and may lead to low blood pressure or infections.
- Intravenous Immunoglobulin (IVIG): IVIG involves the infusion of antibodies from healthy donors to help modulate the immune system. It is often used as a short-term treatment for worsening symptoms or in preparation for surgery.
Monoclonal Antibody Therapy
For patients who do not respond well to traditional immunosuppressants, newer biologic therapies offer targeted treatment options:
- Rituximab (Rituxan) – Originally developed for autoimmune diseases and cancers, this medication reduces B cells, which play a role in antibody production. It is particularly effective for MuSK antibody-positive MG.
- Eculizumab (Soliris) – This drug blocks a specific part of the immune system known as the complement pathway, which is involved in nerve-muscle damage in MG. It is primarily used for AChR antibody-positive generalized MG.
Thymectomy: Surgical Treatment for MG
For some MG patients, thymectomy (surgical removal of the thymus gland) may be recommended. The thymus gland plays a role in the immune system, and in some MG patients, particularly those with AChR antibody-positive MG, removing it may lead to symptom improvement or even remission. A thymectomy is especially recommended if the patient has a thymoma (a tumor of the thymus gland). The procedure can be performed through open surgery or a minimally invasive robotic-assisted approach, leading to reduced recovery time.
Emerging and Experimental Treatments
Ongoing research continues to explore new treatment options for MG:
- New monoclonal antibodies targeting different immune pathways.
- Gene therapy aimed at correcting the underlying autoimmune response.
- Personalized medicine approaches to tailor treatments based on a patient’s specific immune system activity.
While managing MG requires lifelong treatment, advancements in neurological care continue to improve outcomes for patients. By working closely with a neurologist and following a tailored treatment plan, individuals with MG can achieve better symptom control and an improved quality of life.
Lifestyle Adjustments to Manage Myasthenia Gravis
In addition to medical treatments, lifestyle modifications play a crucial role in managing Myasthenia Gravis (MG). Since MG symptoms, such as muscle weakness and fatigue, can fluctuate throughout the day, adopting strategies to conserve energy and optimize daily activities can make a significant difference in overall well-being. Below are some key lifestyle adjustments that can help individuals with MG maintain a higher quality of life.
Energy Conservation Strategies
One of the most common challenges for MG patients is muscle fatigue, which worsens with activity. Learning to conserve energy can help individuals manage symptoms effectively.
- Prioritize tasks: Focus on the most important activities during times of peak energy (e.g., mornings or after rest).
- Take frequent breaks: Avoid prolonged exertion by incorporating rest periods between activities.
- Use assistive devices: Items like grab bars, shower chairs, or electric can openers can reduce strain on weakened muscles.
- Ask for help: Delegate heavy tasks and allow friends or family to assist when needed.
Dietary Considerations
Muscle weakness in the face and throat can make chewing and swallowing difficult. Adjusting one’s diet can help prevent fatigue and choking risks.
- Eat soft, easy-to-chew foods: Mashed potatoes, yogurt, smoothies, and soups can be easier to consume.
- Smaller, more frequent meals: Eating five or six small meals per day instead of three large meals can help maintain energy levels.
- Stay hydrated: Drinking plenty of water aids digestion and prevents dehydration, which can exacerbate fatigue.
- Avoid trigger foods: Hard, crunchy, or dry foods may worsen swallowing difficulties. Alcohol and caffeine should also be limited, as they can contribute to muscle fatigue.
Exercise and Physical Therapy
Although excessive activity can worsen symptoms, gentle, low-impact exercises can help maintain muscle strength without overexertion.
- Work with a physical therapist: A therapist can design a safe, personalized exercise plan.
- Focus on low-impact exercises: Activities like swimming, yoga, or light resistance training can improve muscle function while minimizing fatigue.
- Avoid overexertion: Exercise should be done at a comfortable pace, with plenty of rest breaks.
Stress Management and Mental Health Support
Stress and anxiety can exacerbate MG symptoms, making relaxation and mental health care essential.
- Practice relaxation techniques: Deep breathing exercises, meditation, and mindfulness can help reduce stress.
- Consider therapy or counseling: Speaking with a mental health professional can help manage anxiety or depression related to chronic illness.
- Join a support group: Connecting with others who have MG can provide emotional support and practical advice.
Sleep and Rest Optimization
Since muscle weakness worsens with fatigue, proper rest is essential.
- Follow a regular sleep schedule: Going to bed and waking up at the same time each day can improve sleep quality.
- Use supportive pillows: A slightly elevated head position can aid breathing and prevent discomfort.
- Limit screen time before bed: Reducing blue light exposure from phones and tablets can improve sleep.
By incorporating these lifestyle adjustments, individuals with MG can manage symptoms more effectively and improve their day-to-day functionality. A well-balanced approach that includes both medical treatments and self-care strategies can lead to better long-term outcomes.
Preventing and Managing Myasthenic Crisis
A myasthenic crisis is a severe and potentially life-threatening complication of Myasthenia Gravis (MG), characterized by extreme muscle weakness, particularly in the respiratory muscles, leading to difficulty breathing. Without prompt medical intervention, it can result in respiratory failure. Recognizing early warning signs, understanding emergency treatments, and having a crisis management plan in place can help prevent severe outcomes.
Recognizing Early Warning Signs
Being aware of the early symptoms of a myasthenic crisis allows for timely medical intervention. Some key warning signs include:
- Increasing muscle weakness – Especially in the neck, throat, and respiratory muscles.
- Severe difficulty swallowing (dysphagia) – Risk of choking or aspiration pneumonia.
- Shortness of breath (dyspnea) – Feeling breathless even while at rest.
- Changes in speech – Slurred or nasal-sounding speech due to weakened throat muscles.
- Eyelid drooping and vision problems – Sudden worsening of ptosis (drooping eyelids) and double vision.
If these symptoms escalate, immediate medical attention is required.
Emergency Treatments for Myasthenic Crisis
When a myasthenic crisis occurs, hospitalization is often necessary for respiratory support and medical intervention. Common emergency treatments include:
- Plasmapheresis (Plasma Exchange): Removes harmful antibodies from the bloodstream, providing temporary symptom relief.
- Intravenous Immunoglobulin (IVIG): Provides immune system modulation to reduce symptoms.
- Mechanical Ventilation: In severe cases, a ventilator may be required to assist with breathing.
- Corticosteroids and Immunosuppressants: Used to help control immune system activity and prevent future crises.
How Caregivers Can Assist in Crisis Situations
Caregivers and family members play a crucial role in identifying early signs of crisis and ensuring immediate medical care. Steps they can take include:
- Monitoring breathing patterns: Any sign of difficulty breathing should be taken seriously.
- Keeping emergency contacts accessible: Ensure quick access to a neurologist, emergency services, and the nearest hospital.
- Helping with medication management: Ensuring that medications are taken as prescribed to prevent sudden worsening of symptoms.
- Encouraging rest and energy conservation: Preventing overexertion can help minimize the risk of a crisis.
Long-Term Prevention Strategies
Preventing a myasthenic crisis involves maintaining good overall health and staying on top of treatment plans. Some key strategies include:
- Strict adherence to prescribed medications: Skipping doses or stopping medications suddenly can lead to worsening symptoms.
- Avoiding known triggers: Infections, stress, extreme temperatures, and certain medications (e.g., beta-blockers, certain antibiotics) can provoke an exacerbation.
- Regular check-ups with a neurologist: Monitoring disease progression can help adjust treatments as needed.
- Getting vaccinations: Protecting against respiratory infections like pneumonia and the flu can reduce the risk of complications.
By recognizing early symptoms, understanding emergency treatments, and taking preventive measures, individuals with Myasthenia Gravis can significantly reduce the likelihood of experiencing a myasthenic crisis. Education, preparedness, and proactive care are key to maintaining stability and preventing life-threatening complications.
Conclusion
Managing Myasthenia Gravis requires a multifaceted approach that combines medical treatments with lifestyle modifications to enhance quality of life. While medications, advanced therapies, and, in some cases, surgery can help control symptoms, everyday adjustments such as energy conservation, proper nutrition, stress management, and careful monitoring of triggers are equally essential. Understanding the risks of a myasthenic crisis and having a plan in place can further improve long-term outcomes. By working closely with healthcare providers, staying informed about new treatment options, and making proactive lifestyle choices, individuals with MG can maintain greater independence and overall well-being. Though living with MG presents challenges, with the right strategies, it is possible to lead a fulfilling and active life.





