Most headaches aren’t dangerous. Annoying, yes — but dangerous? Usually not. In fact, the majority of headaches are caused by tension, migraine, illness, stress and a big headache culprit: dehydration.[1] But occasionally, a significant headache can be the nervous system’s way of sounding the alarm that something serious is happening, including a stroke.
That possibility can feel frightening, but understanding what makes a stroke-related headache different can help you respond quickly and appropriately.
Can a Stroke Cause a Headache?
Not all strokes cause headaches, and many stroke symptoms occur without head pain.
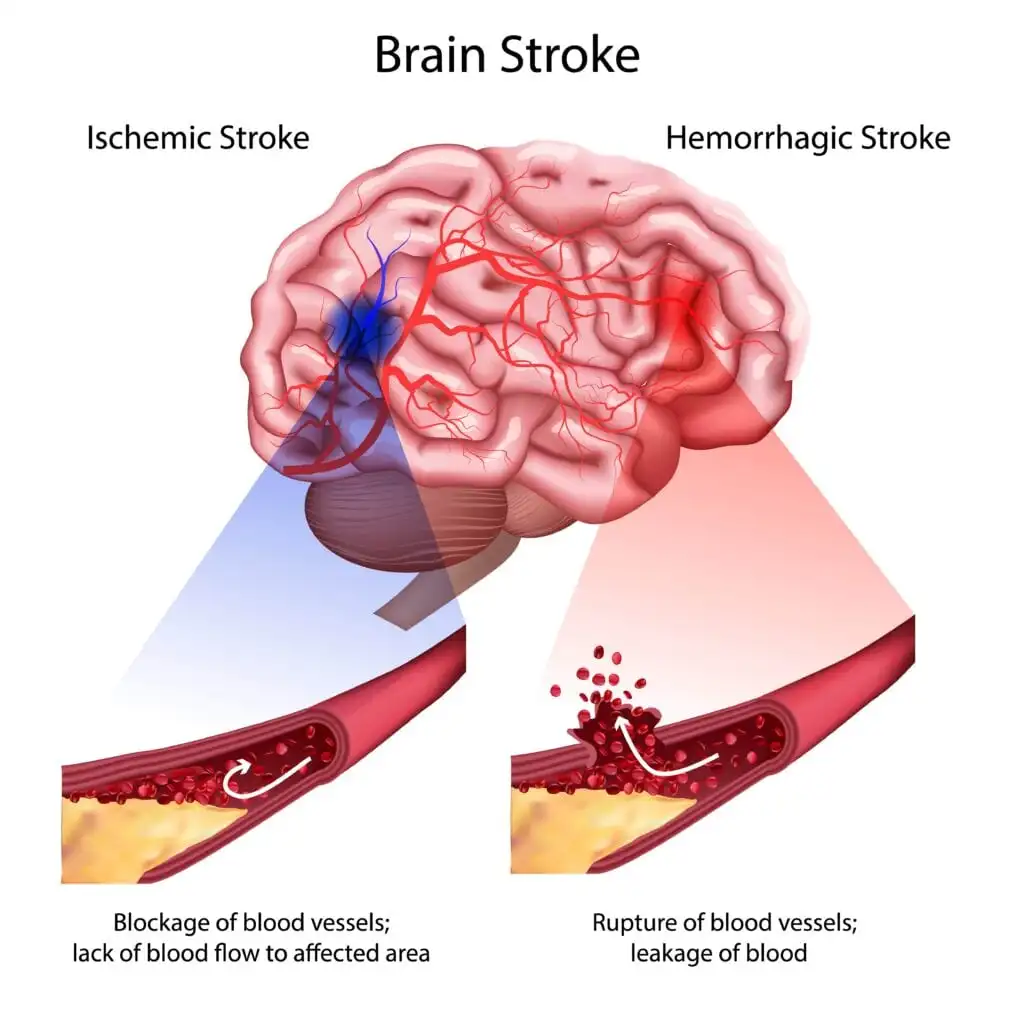
There are two major types of stroke: ischemic stroke, caused by a blocked blood vessel, and hemorrhagic stroke, caused by bleeding in or around the brain.[2] Hemorrhagic strokes are much more likely to cause significant head pain because blood irritates pain-sensitive structures surrounding the brain. [3] Some hemorrhagic strokes happen when a weakened blood vessel in the brain, called an aneurysm, ruptures and causes bleeding around the brain. [4]
Ischemic strokes, which account for most strokes, often occur without headache, which is why sudden neurological symptoms matter even when pain is absent.[5]
When a headache occurs with a stroke, it typically feels very different from a person’s usual headaches. That difference is often the most important clue. This is why sudden, severe headaches matter neurologically. They can signal bleeding, pressure changes, or brain irritation that require immediate medical evaluation.
What Does a Neurological Headache During a Stroke Feel Like?
Patients often describe stroke-related or neurological headaches as unusual, sudden, and intense. Ischemic and hemorrhagic strokes can cause a headache, but how they feel and where you feel it differ.
A sudden onset or sentinel headache may:
- Start suddenly without warning, reaching peak intensity within seconds or minutes. [6]
- Feel like the “worst headache of your life.” [7]
- Be described as explosive or thunderclap-like. [4]
- Feel different from any prior migraine or tension headache. [2]
- Occur along with neck stiffness, nausea, confusion, or decreased alertness, particularly with bleeding around the brain. [8]
Thunderclap headaches are serious because they may signal subarachnoid hemorrhage, a life-threatening type of stroke that requires immediate evaluation.[6]
While migraine headaches can sometimes be severe and sudden, they usually follow a recognizable personal pattern. A headache that feels completely unfamiliar should always be taken seriously.[9]
Because migraine symptoms like severe head pain, visual changes, numbness, or difficulty speaking can overlap with stroke symptoms, sudden or unusual neurological symptoms should always be evaluated. [9]
Stroke Symptoms That Matter More Than the Headache
A headache alone rarely confirms a stroke or medical emergency. Neurologists pay close attention to neurological symptoms that appear suddenly, especially when they occur with head pain.
According to the American Stroke Association, the easiest way to remember stroke warning signs is the
FAST Acronym:
F = Face Drooping
Is one side of your face numb or droopy? Is someone you know showing signs of a stroke? Ask them to smile: if their smile is uneven, they may be experiencing stroke symptoms.
A = Arm Weakness
One arm is weak or numb. Can you raise both arms, or does one arm drift downward when you try?
S = Speech Difficulty
Is the person having trouble speaking? Is their speech slurred?
T = Time to call 911
Don’t hesitate! Every second counts when you think you or someone else is showing signs of a stroke.[10]
Besides a Severe Headache, What Are Other Possible Stroke Symptoms?
Other warning signs of stroke can include sudden vision changes, trouble walking or maintaining balance, confusion, or numbness affecting one side of the body.[3; 10; 11]
When these symptoms appear suddenly, time matters more than certainty. Stroke treatment is most effective when started quickly.[12]
When to Seek Emergency Care for a Headache
It’s the old “better safe than sorry” mantra many of us grew up hearing, and when it comes to sudden or unusual headaches, it still applies. Knowing when to seek medical care can help you respond with confidence instead of fear.
Most headaches are not emergencies. But a headache should be evaluated immediately if it is:
- Sudden and severe
- Completely different from your usual headaches
- Accompanied by neurological symptoms
- Associated with confusion, weakness, or vision changes
The brain doesn’t send many “pain signals,” so when it does, especially suddenly, it’s worth paying attention. Secondary headaches caused by bleeding, vascular problems, or other neurological conditions require urgent care.[7]
If you think a stroke might be happening, it’s always safer to get evaluated.
When a Headache Could Be a Stroke Warning
Most headaches are not strokes. But a sudden, severe, unfamiliar headache, especially with neurological symptoms or F.A.S.T. stroke warning signs, should never be ignored. Knowing the difference between a common headache and a possible stroke warning sign can help you respond with confidence instead of panic.
From a neurologist’s perspective, the biggest concern isn’t how painful a headache is, but how suddenly it starts, how different it feels, and what other neurological symptoms appear alongside it. These clues help your medical team distinguish a typical headache from one that may signal a problem with blood flow or bleeding in the brain.
Trust your instincts. If something feels different or alarming about how your head hurts, don’t blow it off. Seek medical care right away. Acting quickly can help protect vital brain function and, in some cases, save a life.
Disclaimer: This blog is intended for educational and informational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. Always consult your physician, neurologist, or other qualified healthcare provider with any questions you may have regarding a medical condition or treatment. Do not disregard professional medical advice or delay seeking it because of something you read on this blog.
Resources:
- Headache. National Institute of Neurological Disorders and Stroke [Internet]. www.ninds.nih.gov. Published November 22, 2024. Accessed February 13, 2026. Available from: https://www.ninds.nih.gov/health-information/disorders/headache
- Doherty C. Are Headaches a Sign of Stroke? Very Well Health [Internet] Updated December 04, 2025. Accessed February 08, 2026. Available from: https://www.verywellhealth.com/how-a-headache-may-be-a-sign-of-a-stroke-1719596
- Brown R. Stroke. Mayo Clinic [Internet]. Published 2024. Accessed February 13, 2026. Available from: https://www.mayoclinic.org/diseases-conditions/stroke/symptoms-causes/syc-20350113
- Sekhon S, Sharma R, Cascella M. Thunderclap Headache. [Updated 2023 Jun 4]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan-. Accessed February 13, 2026. Available from: https://www.ncbi.nlm.nih.gov/books/NBK560629/
- Diener HS. Headache associated with ischemic cerebrovascular disease. Medlink Neurology, San Diego: Medlink, LLC [Internet]. Updated December 19, 2024. Accessed February 13, 2026. Available from: https://www.medlink.com/articles/headache-associated-with-ischemic-cerebrovascular-disease
- Thunderclap Headaches. Cleveland Clinic [Internet]. Updated October 12, 2022. Accessed February 13, 2026. Available from: https://my.clevelandclinic.org/health/symptoms/17876-thunderclap-headaches
- Dodick DW, Schwedt TJ. OTHER SECONDARY HEADACHE DISORDERS. Clinical Gate [Internet]. Published October 04, 2015. Accessed February 13, 2026. Available from: https://clinicalgate.com/other-secondary-headache-disorders/
- Seifert CL, Schönbach EM, Magon S, et al. Headache in acute ischaemic stroke: a lesion mapping study. Brain: Oxford Academic [Internet]. Volume 139, Issue 1, January 2016, Pages 217–226. https://doi.org/10.1093/brain/awv333. Accessed February 13, 2026. Available from: https://academic.oup.com/brain/article-abstract/139/1/217/2468816
- Migraine and stroke. The Migraine Trust [Internet]. Accessed February 13, 2026. Available from: https://migrainetrust.org/understand-migraine/migraine-and-stroke/
- Stroke Symptoms. American Stroke Association [Internet]. Published 2024. Accessed February 13, 2026. Available from: https://www.stroke.org/en/about-stroke/stroke-symptoms
- Stroke Warning Signs. The Stroke Foundation. [Internet]. Published 2020. Accessed February 13, 2026. Available from: https://www.thestrokefoundation.org/stroke-facts/stroke-warning-signs
- Mayo Clinic Staff. Stroke. Diagnosis and Treatment. Mayo Clinic [Internet]. Accessed February 13, 2026. Available from: https://www.mayoclinic.org/diseases-conditions/stroke/diagnosis-treatment/drc-20350119

