About Multiple Sclerosis Treatments in Stuart FL
Multiple sclerosis (MS) is a demyelinating disease in which the myelin sheath which is the covering of the brain and spinal cord gets damaged. This damage disrupts the ability of parts of the nervous system to communicate, resulting in a wide range of signs and symptoms including abnormal sensation, muscle weakness, mental and sometimes psychiatric problems. We offer professional Multiple Sclerosis treatments in Stuart Florida and can help you find the best medications for your specific health care needs.
Prevalence estimates for MS in the United States is around 70-95 per 100,000 population according to different studies. According to the National Multiple Sclerosis Society, around 400,000 individuals in the United States are affected by MS. It is more common in women with female-to-male ratio of MS incidence about 2 to 1 ratio. The average age of MS diagnosis is 30 year old, however, it can occur in persons of any age. MS is more common in people who live farther from the equator and in North Europe.
At Premier Neurology Center we offer the best Multiple Sclerosis treatments in Stuart, FL.
Causes:
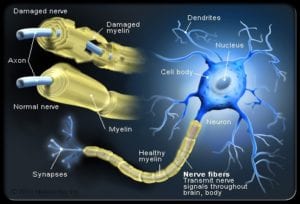
While the cause is not clear, the underlying mechanism is thought to be autoimmune where the immune system attacks and destroy the myelin in the brain and spinal cord disrupting the ability of parts of the nervous system to communicate causing weakness, numbness and other related symptoms.
It has been hypothesized based on many studies that MS results when an environmental agent or event (viral or bacterial infection, exposure to chemicals, etc) acts in concert with a genetic predisposition to immune dysfunction. Low levels of vitamin D have also been proposed as one environmental factor contributing to the development of MS.
Signs and Symptoms:
The signs and symptoms of MS vary tremendously from one person to another with autonomic, visual, motor, and sensory problems being the most common. The specific symptoms are determined by the locations of the lesions within the nervous system. Most people experience their first symptoms of MS between the ages of 20 and 40.
The initial symptom of MS is often blurred or double vision, red-green color distortion, or even blindness in one eye (optic neuritis). Most MS patients experience muscle weakness in their extremities and difficulty with coordination and balance. These symptoms may be severe enough to impair walking or even standing. Most people with MS also exhibit paresthesias, transitory abnormal sensory feelings such as numbness, prickling, or “pins and needles” sensations, difficulties with coordination and balance (ataxia); problems with speech or swallowing and some may also experience pain. Approximately half of all people with MS experience cognitive impairments such as difficulties with concentration, attention, memory, and poor judgment, but such symptoms are usually mild and are frequently overlooked. Depression is another common feature of MS. The main measure of disability and severity is the expanded disability status scale (EDSS), with other measures such as the multiple sclerosis functional composite being increasingly used in research.
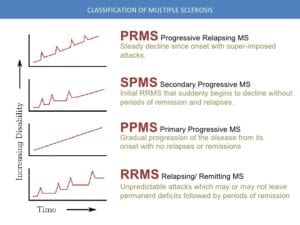 The condition begins in most cases as a clinically isolated syndrome over a number of days with motor or sensory problems. Relapses are usually not predictable, occurring without any warning and preceded by common triggers such as viral infections (common cold, influenza, etc) and they occur more frequently during spring and summer. Several phenotypes (commonly named types), or patterns of progression, have been described:
The condition begins in most cases as a clinically isolated syndrome over a number of days with motor or sensory problems. Relapses are usually not predictable, occurring without any warning and preceded by common triggers such as viral infections (common cold, influenza, etc) and they occur more frequently during spring and summer. Several phenotypes (commonly named types), or patterns of progression, have been described:
- Relapsing-Remitting MS (RRMS)
- Secondary Progressive MS (SPMS)
- Primary Progressive MS (PPMS)
- Progressive Relapsing MS (PRMS)
The Relapsing-Remitting subtype is characterized by unpredictable relapses followed by periods of months to years of relative quiet (remission) with no new signs of disease activity.
Secondary Progressive MS occurs in majority of those with initial relapsing-remitting MS, who eventually have progressive neurologic decline between acute attacks without any definite periods of remission.
The Primary Progressive subtype occurs in about one-fourth of patients, with no remission after the initial symptoms. It is characterized by progression of disability from onset, with minor remissions and improvements.
Progressive Relapsing MS is the least common of all subtypes and describes those individuals who, from onset, have a steady neurologic decline but also have clear superimposed relapses or attacks.
Multiple Sclerosis Doctors in Stuart & Treatment Options:
Patients with signs and symptoms that correlate to MS must have a brain MRI with and without contrast along with other laboratory tests (blood and spinal fluid) must also be ordered to confirm the diagnosis and to rule out other etiologies. Our Multiple Sclerosis doctors in Stuart Florida understand how to properly diagnose, and treat this disease.
Once a diagnosis is made, the decision to start a medication will be discussed between the patient and the neurologist. Although there is no known cure for multiple sclerosis, several therapies have proven helpful. The primary goals of therapy are returning function after an attack or relapse, preventing new relapses, and preventing further disability. As with any medical treatment, medications used in the management of MS have several adverse effects. During symptomatic or acute attacks, administration of high doses of intravenous corticosteroids, such as methylprednisolone, is the usual therapy. While steroids do not affect the course of MS over time, they can reduce the duration and severity of attacks in some patients.
The beta interferons (Avonex, Betaseron, and Rebif) has been shown to reduce the number of relapses and may slow the progression of physical disability. When attacks do occur, they tend to be shorter in duration and less severe. The FDA also has approved a synthetic form of myelin basic protein, called copolymer-I (Copaxone), for the treatment of relapsing-remitting MS. Copolymer-I has few side effects, and studies indicate that the agent can reduce the relapse rate by almost one third. Other FDA approved drugs to treat relapsing forms of MS in adults include teriflunomide and dimethyl fumarate. An immunosuppressant treatment, Novantrone (mitoxantrone), is approved by the FDA for the treatment of advanced or chronic MS. The FDA has also approved dalfampridine (Ampyra) to improve walking and ambulation in individuals with MS.
One monoclonal antibody, natalizumab (Tysabri), is indicated as monotherapy for MS to delay the accumulation of physical disability and reduce the frequency of clinical exacerbations in patients with severe MS and who have failed other medications.
Spasticity, which can occur either as a sustained stiffness caused by increased muscle tone or as spasms that come and go, is usually treated with muscle relaxants such as baclofen, tizanidine, diazepam or clonazepam. Physical therapy and exercise can help preserve remaining function, and patients may find that various aids such as foot braces, canes, and walkers — can help them remain independent and mobile. Other drugs that address depression or fatigue are also used in some patients if needed.
Resources
Multiple Sclerosis Association of America
www.mymsaa.org
Tel: 856-488-4500
Multiple Sclerosis Foundation
www.msfocus.org
Tel: 954-776-6805
National Multiple Sclerosis Society
www.nationalmssociety.org
Tel: 800-344-4867
Citations
NINDS: National Institute of Neurological Disorders and Stroke
URL:
https://www.ninds.nih.gov/Disorders/All-Disorders/Multiple-Sclerosis-Information-Page
Updated July 17, 2015. Accessed October 17, 2015.
Luzzio, Christopher. “Multiple Sclerosis”: Practice Essentials, Background, Pathophysiology. Medscape, updated 14 Oct. 2015. Accessed 19 Oct. 2015.
URL: emedicine.medscape.com/article/1146199-overview



